Comparison of clinical outcomes of implantable collamer lens versus femtosecondlaser in situ keratomileusis and small incision lenticule extraction for moderate-to-high myopia and myopic astigmatism correction
Abstract
Purpose: To compare safety, efficacy, stability, and predictability of implantable collamer lens (ICL) with femtosecond-laser in situ keratomileusis (FS-LASIK) or small incision lenticule extraction (SMILE) for the correction of moderate-to-high myopia/myopic astigmatism.
Study design: We retrospectively collected data from patients with moderate-to-high myopia/myopic astigmatism (spherical equivalent [SE] ≥ −3.00 diopters [D]) who underwent ICL (48 eyes), FS-LASIK (36 eyes), or SMILE (86 eyes) at Hai Yen Eye Center from October 2016 to February 2018.
Materials and methods: The Wilcoxon Mann-Whitney U test was used to compare pre- and postoperative patients’ characteristics of ICL with SMILE or FS-LASIK. Generalized linear models with unstructured correlation matrix and robust standard errors were used to analyze efficacy and safety indices; logistic regression was used for cylinder predictability.
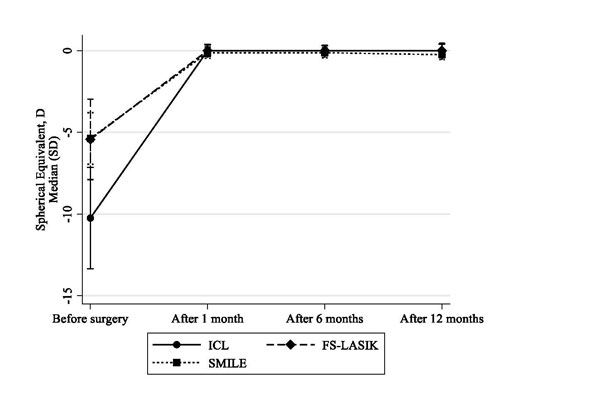
Results: After controlling for age, preoperative SE, and preoperative corrected distance visual acuity (pCDVA), SMILE had significantly lower safety indices (Coefficient = −0.04, 95% CI = −0.07–−0.01) and efficacy indices (Coefficient = −0.10, 95% CI = −0.20–−0.01) than did ICL, while FS-LASIK was not significantly different from ICL (Coefficient = −0.02, 95% CI = −0.06–0.02 and Coefficient = −0.01, 95% CI= −0.10–0.09, respectively). ICL SEs
were stable over 12 months after surgery. However, in FS-LASIK and SMILE, SEs significantly decreased at 12 months compared with 6 months after surgery. The percentage of eyes that underwent FS-LASIK and had target SEs within ±0.5 D at 12 months was significantly lower than those that underwent ICL (OR = 0.14, 95% CI = 0.02–0.85), after controlling for age, preoperative SE, and pCDVA.
Conclusion: For the correction of moderate-to-high myopia/myopic astigmatism, ICL seems to perform better than SMILE and FS-LASIK.
References
Reinstein DZ, Archer TJ, Gobbe M. Small incision lenticule extraction (SMILE) history, fundamentals of a new refractive surgery technique and clinical outcomes. Eye Vis (Lond). 2014;1:3. Epub 2014/01/01. https://doi.org/10.1186/s40662-014-0003-1. PubMed PMID: 26605350; PubMed Central PMCID: PMCPMC4604118.
Huang D, Schallhorn SC, Sugar A, et al. Phakic intraocular lens implantation for the correction of myopia: a report by the American Academy of Ophthalmology. Ophthalmology. 2009;116(11):2244-2258. Epub 2009/11/04. https://doi.org/10.1016/j.ophtha.2009.08.018. PubMed PMID: 19883852.
Lee J, Kim Y, Park S, et al. Long-term clinical results of posterior chamber phakic intraocular lens implantation to correct myopia. Clin Exp Ophthalmol. 2016;44(6):481-487. https://doi.org/10.1111/ceo.12691. PubMed PMID: 26661832.
Chang J, Lau S. Toric Implantable Collamer Lens for high myopic astigmatic Asian eyes. Ophthalmology. 2009;116(12):2340-2347. https://doi.org/10.1016/j.ophtha.2009.04.053. PubMed PMID: 19744727.
Dougherty PJ, Priver T. Refractive outcomes and safety of the implantable collamer lens in young low-to-moderate myopes. Clin Ophthalmol. 2017;11:273-277. https://doi.org/10.2147/OPTH.S120427. PubMed PMID: 28203053; PubMed Central PMCID: PMCPMC5298816.
Han T, Xu Y, Han X, et al. Three-year outcomes of small incision lenticule extraction (SMILE) and femtosecond laser-assisted laser in situ keratomileusis (FS-LASIK) for myopia and myopic astigmatism. Br J Ophthalmol. 2019;103(4):565-568. Epub 2018/08/01. https://doi.org/10.1136/bjophthalmol-2018-312140. PubMed PMID: 30061116.
Li M, Li M, Chen Y, et al. Five-year results of small incision lenticule extraction (SMILE) and femtosecond laser LASIK (FS-LASIK) for myopia. Acta Ophthalmol. 2019;97(3):e373-e380. Epub 2019/01/12. https://doi.org/10.1111/aos.14017. PubMed PMID: 30632671.
Liu M, Chen Y, Wang D, et al. Clinical Outcomes After SMILE and Femtosecond Laser-Assisted LASIK for Myopia and Myopic Astigmatism: A Prospective Randomized Comparative Study. Cornea. 2016;35(2):210-216. Epub 2015/12/20. https://doi.org/10.1097/ICO.0000000000000707. PubMed PMID: 26684046.
Yan H, Gong LY, Huang W, Peng YL. Clinical outcomes of small incision lenticule extraction versus femtosecond laser-assisted LASIK for myopia: a Meta-analysis. Int J Ophthalmol. 2017;10(9):1436-1445. Epub 2017/09/26. https://doi.org/10.18240/ijo.2017.09.17. PubMed PMID: 28944205; PubMed Central PMCID: PMCPMC5596231.
Kang P, Gifford P, McNamara P, et al. Peripheral refraction in different ethnicities. Invest Ophthalmol Vis Sci. 2010;51(11):6059-6065. Epub 2010/05/28. https://doi.org/10.1167/iovs.09-4747. PubMed PMID: 20505193.
Twelker JD, Mitchell GL, Messer DH, et al. Children’s Ocular Components and Age, Gender, and Ethnicity. Optom Vis Sci. 2009;86(8):918-935. Epub 2009/08/04. PubMed PMID: 19650241; PubMed Central PMCID: PMCPMC2901932.
Ganesh S, Brar S, Pawar A. Matched population comparison of visual outcomes and patient satisfaction between 3 modalities for the correction of low to moderate myopic astigmatism. Clin Ophthalmol. 2017;11:1253-1263. https://doi.org/10.2147/OPTH.S127101. PubMed PMID: 28740361; PubMed Central PMCID: PMCPMC5505606.
Kamiya K, Shimizu K, Igarashi A, Hikita F, Komatsu M. Four-year follow-up of posterior chamber phakic intraocular lens implantation for moderate to high myopia. Arch Ophthalmol. 2009;127(7):845-850. Epub 2009/07/15. https://doi.org/10.1001/archophthalmol.2009.67. PubMed PMID: 19597102.
Yo C, Vroman C, Ma S, Chao L, McDonnell PJ. Surgical outcomes of photorefractive keratectomy and laser in situ keratomileusis by inexperienced surgeons. J Cataract Refract Surg. 2000;26(4):510-515. https://doi.org/10.1016/s0886-3350(99)00468-x. PMID: 10771223.
Copyright (c) 2021 Yen Hai Tran, Huy Dinh Minh Tran, Ly Thi-Hai Tran, Dung Thi Mong Nguyen, Chuong Nguyen Thao Le, Thanh Cong Bui

This work is licensed under a Creative Commons Attribution 4.0 International License.
Authors who publish with this journal agree to the following terms:
- Authors retain copyright and grant the journal right of first publication, with the work twelve (12) months after publication simultaneously licensed under a Creative Commons Attribution License that allows others to share the work with an acknowledgement of the work's authorship and initial publication in this journal.
- Authors are able to enter into separate, additional contractual arrangements for the non-exclusive distribution of the journal's published version of the work (e.g., post it to an institutional repository or publish it in a book), with an acknowledgement of its initial publication in this journal.
- Authors are permitted and encouraged to post their work online (e.g., in institutional repositories or on their website) prior to and during the submission process, as it can lead to productive exchanges, as well as earlier and greater citation of published work (See The Effect of Open Access).


