Retinal thickness among normal myopic Filipinos using spectral domain optical coherence tomography
Abstract
Purpose: To determine mean macular and retinal nerve fiber layer (RNFL) thickness of myopic Filipinos using spectral domain optical coherence tomography (SD-OCT) and to evaluate influence of age, gender, and degree of myopia.
Design: Observational clinic-based cohort.
Methods: Participants were divided into two groups: low-moderate myopia [spherical equivalent (SE) -0.50 D to -6.00 D] and high-pathologic myopia (SE < -6.00 D and AL > 26.5 mm). Subgroup analyses between low myopia (refraction < -3.00 D or less) and moderate myopia (> -3.00 D to -6.00 D), and high myopia (> -6.00 D to -8.00 D) and pathologic myopia (more than -8.00 D) were done. Macular and RNFL thickness were measured by a SD-OCT and axial length (AL) with non-contact biometry.
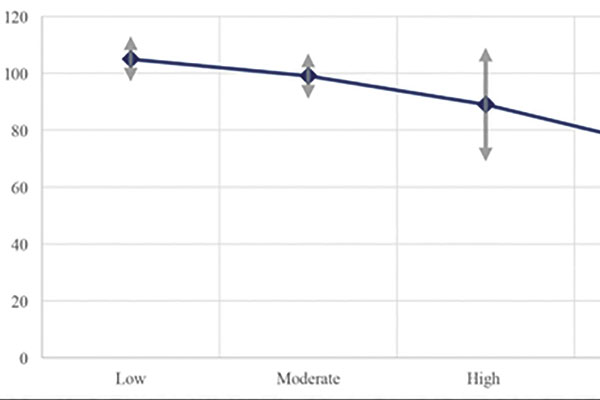
Results: Of 156 eyes, 88/156 (56%) had low-moderate myopia, 68/156 (44%) had high-pathologic myopia. There were 67/156 (43%) male and 89/156 (57%) female subjects. Mean central foveal subfield thickness measurements were 264 ± 24 μm for low myopia, 258 ± 17 μm for moderate myopia, 253 ± 25 μm for high myopia, and 218 ± 48 μm for pathologic myopia. Mean RNFL thickness measurements were 105.62 ± 3.89 μm
for low myopia, 97.6 ± 2.45 μm for moderate myopia, 85.9 ± 3.87 μm for high myopia, and 75.14 ± 3.89 μm for pathologic myopia. Average SE (p < 0.0001) decreased while AL (p < 0.0001) increased with more myopia. Myopia and age significantly affected macular and RNFL thickness parameters except for the following where only the degree of myopia was a significant factor: central foveal, temporal parafoveal, nasal perifoveal, inferior and nasal RNFL thicknesses.
Conclusion: Retinal SD-OCT thickness measurements decreased with increasing level of myopia and age. Central foveal, temporal parafoveal, nasal perifoveal, inferior and nasal RNFL thicknesses may be more appropriate SD-OCT parameters among myopic Filipino patients to monitor for glaucoma since they may be less influenced by age.
References
Wang Q, Klein BE, Klein R, Moss SE. Refractive status in the Beaver Dam Eye Study. Invest Ophthalmol Vis Sci. 1994;35:4344-4347. https://www.ncbi.nlm.nih.gov/pubmed/8002254.
Zhao J, Pan X, Sui R, Munoz SR, Sperduto RD, Ellwein LB. Refractive error study in children: results from Shunyi District, China. Am J Ophthalmol. 2000;129:427-435. https://www.ncbi.nlm.nih.gov/pubmed/10764849
Lin LL, Shih YF, Hsiao CK, Chen CJ, Lee LA, Hung PT. Epidemiologic study of the prevalence and severity of myopia among schoolchildren in Taiwan in 2000. J Formos Med Assoc. 2001;100:684-691. https://www.ncbi.nlm.nih.gov/pubmed/11760374.
Ling SL, Chen AJ, Rajan U, Cheah WM. Myopia in ten year old children—a case control study. Singapore Med J. 1987;28:288-292. https://www.ncbi.nlm.nih.gov/pubmed/3423791.
Reyes KB, Uy HS. Refractive errors in Filipino eyes in a single-center study population. Philipp J Ophthalmol. 2010;35:50-55. paojournal.com/vol35no2/toc.php.
Kang SH, Hong, SW, Im SK, Lee SH, Ahn MD. Effect of myopia on the thickness of the retinal nerve fiber layer measured by Cirrus HD optical coherence tomography. Invest Ophthalmol Vis Sci. 2010;51:4075-4083. https://www.ncbi.nlm.nih.gov/pubmed/20237247.
Foster PJ, Jiang Y. Epidemiology of myopia. Eye (Lond). 2014;28:202-208. https://www.ncbi.nlm.nih.go/pubmed/24406412.
Emerole CG, Nneli RO, Osim EE. Prevalence, distribution and determinants of myopia in Owerri, Nigeria. J Exp Clin Anat. 2013;12: 57-61. http://www.jecajournal.org/article.asp?issn=1596-2393;year=2013;volume=12;issue=2;spage=57;epage=61;aulast=Emerole.
Saw SM, Gazzard G, Shi-Yen E, Chua WH. Myopia and associated pathological complications. Ophthal Physio Opt. 2005;25:381-391. https://www.ncbi.nlm.nih.gov/pubmed/16101943.
Shoji T, Sato H, Ishida M, Takeuchi M, Chihara E. Assessment of glaucomatous changes in subjects with high myopia using spectral domain optical coherence tomography. Invest Ophthalmol Vis Sci. 2011;52:1098-1102. https://www.ncbi.nlm.nih.gov/pubmed/21051712.
Akashi A, Kanamori A, Ueda K, Inoue Y, Yamada Y, Nakamura M. The ability of SD-OCT to differentiate early glaucoma with high myopia from highly myopic controls and non-highly myopic control. Invest Ophthalmol Vis Sci. 2015;56:6573-6580. https://iovs.arvojournals.org/article.aspx?articleid=2464683.
Holden B, Fricke T, Wilson D, et al. Global prevalence of myopia and high myopia and temporal trends from 2000 through 2050. Am J Ophthalmol. 2016;123:1036-1042. https://www.ncbi.nlm.nih.gov/pubmed/26875007.
Jonas JB, Xu L. Histological changes of high axial myopia. Eye. 2014;28:113-117. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3930258.
Beresford J, Crewther S, Kiely P, Crewther DP. Comparison of refractive state and circumferential morphology of retina, choroid and sclera in chick models of experimentally induced ametropia. Optom Vis Sci. 2002;78:40-49. https://www.ncbi.nlm.nih.gov/pubmed/11233334.
Grover S, Murthy R, Brar V, Chalam KV. Normative data for macular thickness by high-definition spectral-domain optical coherence tomography (Spectralis®). Am J Ophthalmol. 2009;148:266-271. https://www.ncbi.nlm.nih.gov/pubmed/19427616.
Kanai K, Abe T, Murayama K, Yoneya S. Retinal thickness and changes with age. Nippon Ganka Gakkai Zasshi. 2002;106:162-165. https://www.ncbi.nlm.nih.gov/pubmed/11925953.
Chan A, Duker JS, Ko TH, Fujimoto JG, Schuman JS. Normal macular thickness measurements in healthy eyes using Stratus optical coherence tomography. Arch Ophthalmol. 2006;124:193-198. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1941772/.
Copyright (c) 2020 Camille Elaine Zabala, Jubaida Mangondato-Aquino, Jose Ma. Martinez, John Mark de Leon

This work is licensed under a Creative Commons Attribution 4.0 International License.
Authors who publish with this journal agree to the following terms:
- Authors retain copyright and grant the journal right of first publication, with the work twelve (12) months after publication simultaneously licensed under a Creative Commons Attribution License that allows others to share the work with an acknowledgement of the work's authorship and initial publication in this journal.
- Authors are able to enter into separate, additional contractual arrangements for the non-exclusive distribution of the journal's published version of the work (e.g., post it to an institutional repository or publish it in a book), with an acknowledgement of its initial publication in this journal.
- Authors are permitted and encouraged to post their work online (e.g., in institutional repositories or on their website) prior to and during the submission process, as it can lead to productive exchanges, as well as earlier and greater citation of published work (See The Effect of Open Access).


