Is there variable neuronal susceptibility to compression?
A case report of differential recovery from dorsal midbrain syndrome and compressive optic neuropathy following treatment for germinoma
Abstract
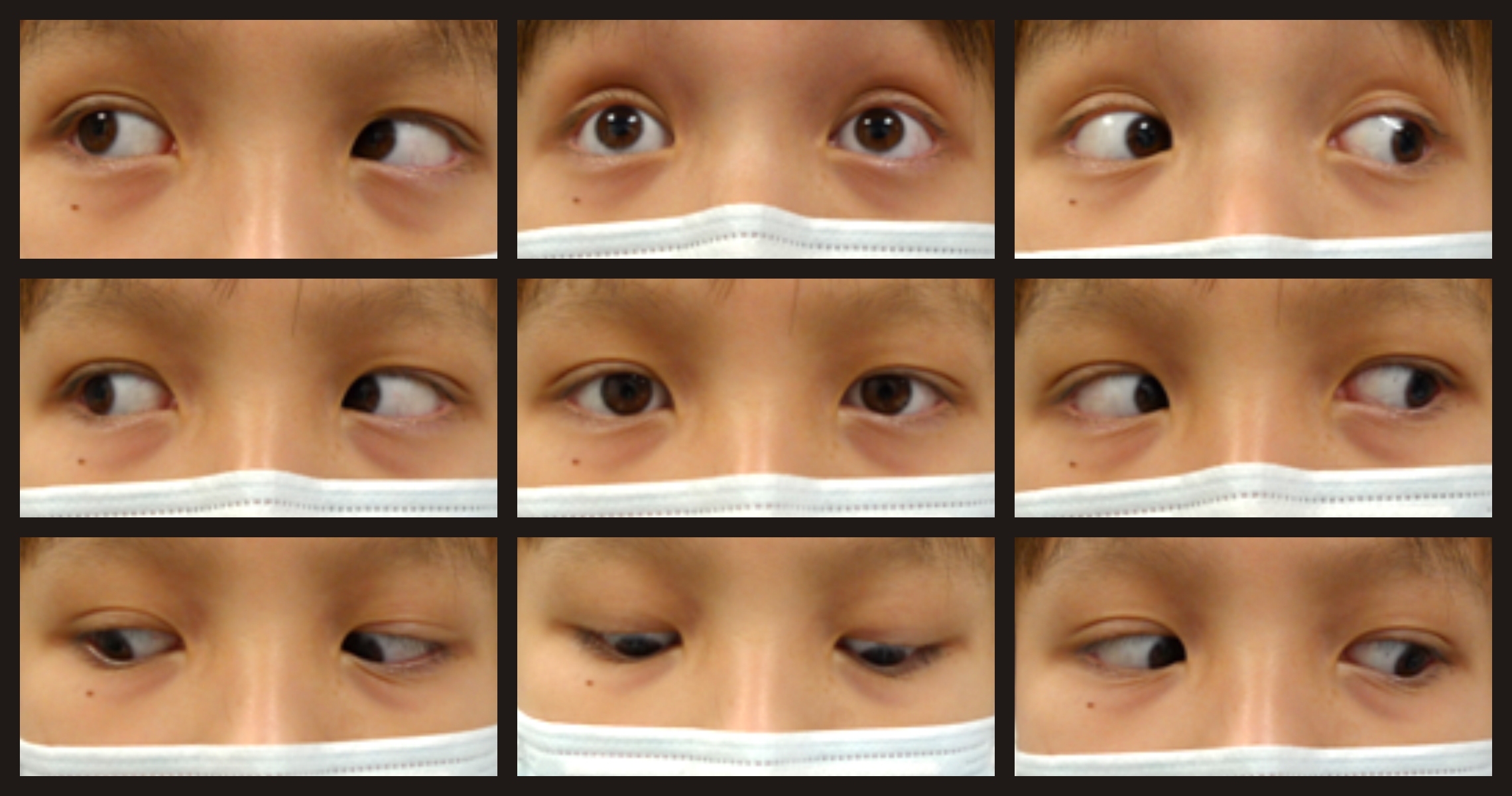
A 12-year-old boy with suprasellar germinoma complicated by hydrocephalus was found to have dorsal midbrain syndrome and bilateral compressive optic neuropathy. Following a third ventricular neuroendoscopic biopsy and the initiation of chemotherapy, a follow-up magnetic resonance imaging scan of the brain showed significant regression of the tumor with resolution of hydrocephalus. On smooth pursuit, there was significant improvement in upgaze. However, light-near dissociation of his pupillary defect was persistent. Fundal examination showed persistent temporal pallor of the optic discs bilaterally, associated with a suboptimal best-corrected visual acuity of 20/40 and bilateral centrocecal scotoma.The differential recovery of neuronal function following relief of compression is poorly understood. In this case, both the optic nerve and pretectal axonal fibers responsible for pupillary reflex, with their neuronal cell bodies residing outside the direct compressive site at the midbrain, showed poor functional recovery. However, relief of pressure at the rostral interstitial medial longitudinal fasciculus and posterior commissure nuclear complexes resulted in significant clinical improvement in upgaze.
This case suggests that, for neurons, axons are apparently more susceptible to pressure than cell bodies. The predominant transmission of nerve impulses takes place through the length of axons, and thus is more sensitive to pressure changes, with the associated microvascular compromise and demyelination.
References
treatment and tumor response. Ital J Neurol Sci. 1987;8(3):267-270.
2. Baloh RW, Furman JM, Yee RD. Dorsal midbrain syndrome: clinical and oculographic findings.
Neurology. 1985;35:54-60.
3. Keane JR. The pretectal syndrome: 206 patients. Neurology. 1990;40:684-690.
4. Pierrot-Deseilligny CH, Chain F, Gray F, Serdaru M, Escourolle R, Lhermitte F. Parinaud’s syndrome:
electro-oculographic and anatomical analyses of six vascular cases with deductions about
vertical gaze organization in the premotor structures. Brain. 1982;105(Pt 4):667-696.
5. Corbett JJ. Neuro-ophthalmologic complications of hydrocephalus and shunting procedures.
Semin Neurol. 1986;6(2):111-123.
6. Chattha A, DeLong G. Sylvian aqueduct syndrome as a sign of acute obstructive hydrocephalus
in children. J Neurol Neurosurg Psychiatry. 1975;38:288-296.
7. Bergsneider M, Peacock WJ, Mazziotta JC, Becker DP. Beneficial effect of siphoning in treatment
of adult hydrocephalus. Arch Neurol. 1999;56(10):1224-1229.
Copyright (c) 2019 Asian Journal of Ophthalmology

This work is licensed under a Creative Commons Attribution 4.0 International License.
Authors who publish with this journal agree to the following terms:
- Authors retain copyright and grant the journal right of first publication, with the work twelve (12) months after publication simultaneously licensed under a Creative Commons Attribution License that allows others to share the work with an acknowledgement of the work's authorship and initial publication in this journal.
- Authors are able to enter into separate, additional contractual arrangements for the non-exclusive distribution of the journal's published version of the work (e.g., post it to an institutional repository or publish it in a book), with an acknowledgement of its initial publication in this journal.
- Authors are permitted and encouraged to post their work online (e.g., in institutional repositories or on their website) prior to and during the submission process, as it can lead to productive exchanges, as well as earlier and greater citation of published work (See The Effect of Open Access).


