A peculiar case of corneal autograft in a patient with bilateral advanced glaucoma
Abstract
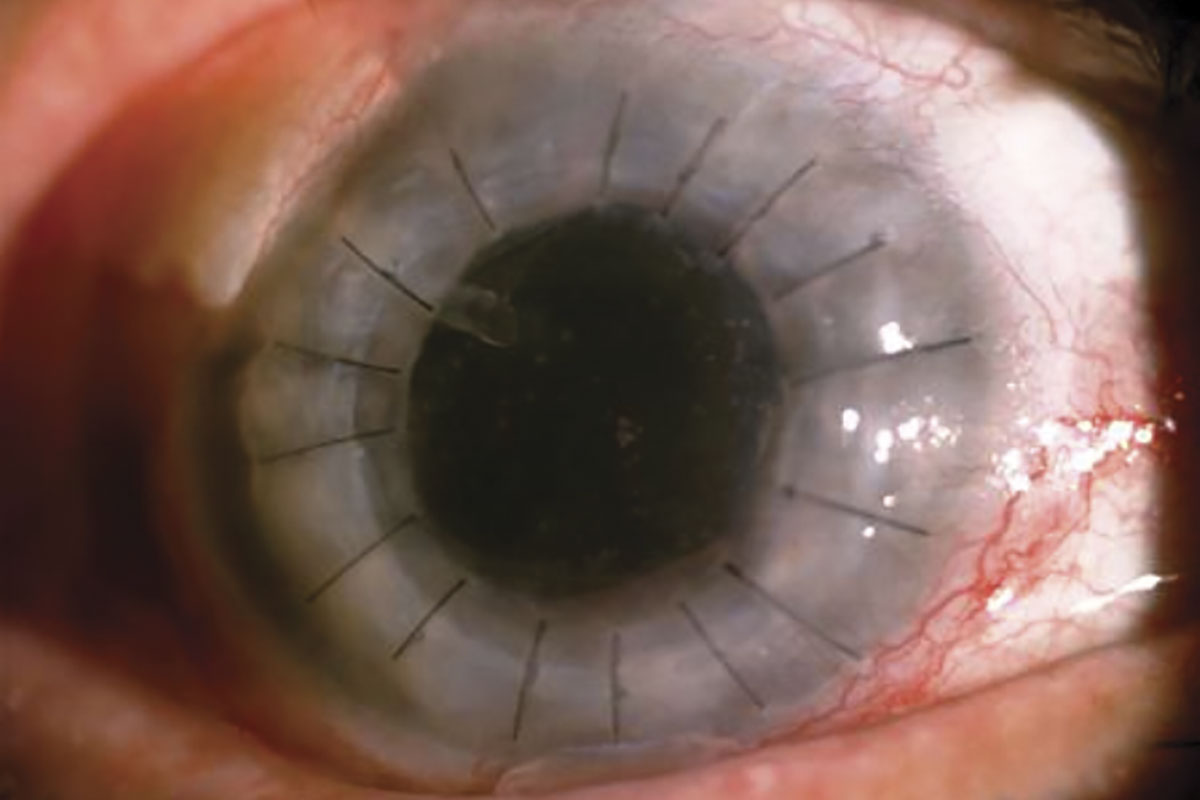
The technique of autograft employs the use of a clear corneal graft from an otherwise blind eye that is transplanted to the fellow eye, which has a visual potential in the same patient. A patient with advanced glaucoma in both eyes presented to us with pseudophakic bullous keratopathy with Ahmed glaucoma valve in the right eye, and cataract and patent peripheral iridotomy with no perception of light in the left eye. The autograft and allograft corneas for bilateral penetrating keratoplasty (PK) were obtained from the contralateral eye and a cadaver eye, respectively. Central corneal button was used for PK. One year after the surgery, the graft host junction was well apposed with no vascularization, corneal surface was clear, sutures were intact, and best corrected visual acuity improved in right eye to 1 logMAR. Bilateral simultaneous PK with autograft in one eye and allograft in the other was done to decrease the chances of rejection.
References
Günes A, Kansu Bozkurt T, Unlu C, Sezgin Akcay BI, Bayramlar H. Ipsilateral rotational autokeratoplasty for the management of traumatic corneal scar. Case Rep Ophthalmol Med. 2012;2012:853584.
Dua HS, Azuara-Blanco A. Corneal allograft rejection: risk factors, diagnosis, prevention, and treatment. Indian J Ophthalmol. 1999;47(1):3.
Arentsen JJ. Corneal transplant allograft reaction: possible predisposing factors. Trans Am Ophthalmol Soc. 1983;81:361-402.
Stewart RM, Jones MN, Batterbury M, et al. Effect of glaucoma on corneal graft survival according to indication for penetrating keratoplasty. Am J Ophthalmol. 2011;151(2):257-262.
Boisjoly HM, Bernard PM, Dubé I, Laughrea PA, Bazin R, Bernier J. Effect of factors unrelated to tissue matching on corneal transplant endothelial rejection. Am J Ophthalmol. 1989;107:647-654.
Khodadoust AA. The allograft rejection: the leading cause of graft failure of clinical corneal grafts. In: Porter R, Knight J, eds. Corneal graft failure. Amsterdam: Associated Scientific Publishers; 1973:151-167 (Ciba Foundation Symposium; 15).
Copyright (c) 2019 Vipul Bhandari, Sri Ganesh, Sneha Thapliyal

This work is licensed under a Creative Commons Attribution 4.0 International License.
Authors who publish with this journal agree to the following terms:
- Authors retain copyright and grant the journal right of first publication, with the work twelve (12) months after publication simultaneously licensed under a Creative Commons Attribution License that allows others to share the work with an acknowledgement of the work's authorship and initial publication in this journal.
- Authors are able to enter into separate, additional contractual arrangements for the non-exclusive distribution of the journal's published version of the work (e.g., post it to an institutional repository or publish it in a book), with an acknowledgement of its initial publication in this journal.
- Authors are permitted and encouraged to post their work online (e.g., in institutional repositories or on their website) prior to and during the submission process, as it can lead to productive exchanges, as well as earlier and greater citation of published work (See The Effect of Open Access).


